DHN Bureau Listens to Patients on India's Digital Health Journey: 100+ Patients with One Clear Message

A ground-level survey of 100+ patients across India's city tiers reveals a healthcare system at a digital inflection point; brimming with promise, burdened by unresolved trust and equity gaps.
India's digital health story is rarely told from the patient's chair. Policymakers chart ambitious trajectories, Ayushman Bharat Digital Mission, ABHA health IDs, and telemedicine frameworks, while entrepreneurs build the infrastructure of tomorrow's hospital. But what does a 34-year-old in Nagpur actually feel when the OTP never arrives? What does a grandmother in a Tier 3 town do when the doctor's face freezes mid-sentence on a patchy video call?
To answer these questions, the DHN Bureau conducted a structured patient experience survey across age groups (18 to 60+), city tiers (Metro to Tier 3/Rural), and healthcare settings (government, private, corporate chains, and local clinics) for a month in Mar 2026. The responses, candid, occasionally blunt, sometimes hopeful, paint a picture that neither triumphant press releases nor skeptical op-eds fully capture. What follows is simply what patients told us.
Data Privacy Being the Loudest in the Room
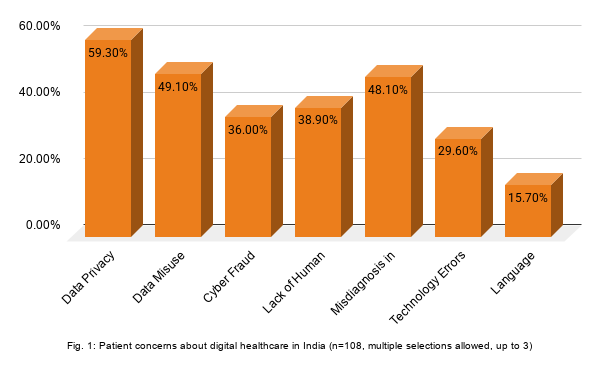
Source: DHN Bureau Patient Survey 2026
If there is one theme that cuts across every age group, city tier, and hospital type in this survey, it is trust, or more precisely, its absence. Data privacy was the single most cited concern in our survey, flagged by nearly two-thirds of respondents. Data misuse and cyber fraud followed closely.
One respondent articulated it with unusual clarity:
"When I researched health insurance for my parents, many companies reached out to me despite not giving my number anywhere. So if I share my health details, I don't know how they will be misusing it."
Of 100+ survey respondents, nearly 3 in 5 (59.3%) flagged data privacy as their primary concern with digital healthcare, making it the single most cited worry by a significant margin. Close behind, data misuse (49.1%) and misdiagnosis in teleconsultation (48.1%) round out the top three, forming a trust triangle that sits at the heart of patient hesitation. Cyber fraud (38%) and lack of human interaction (38.9%) follow almost neck-and-neck, suggesting patients aren't just worried about being hacked; they're equally anxious about being depersonalised.
Technology errors, cited by nearly 1 in 3 (29.6%), reflect a system that patients find unreliable enough to factor into their healthcare decisions actively. Language barriers, at 15.7%, may appear modest in percentage terms, but represent a structural exclusion issue that disproportionately affects rural and older populations whose voices are already underrepresented in surveys like this one.
There is also a quieter but important concern about diagnostic trust. Roughly 60% of respondents said they would use teleconsultation "only for minor issues." The fear of misdiagnosis in teleconsultation was among the top five concerns overall, and several participants explicitly mentioned the difficulty of conveying symptoms through a screen.
The implication for digital health leaders is significant: until AI-assisted diagnostics can meaningfully replicate the reassurance of a physical examination, teleconsultation will remain a first-filter tool. Building patient trust in digital diagnosis is the defining clinical challenge of the next five years.
What Makes Patients Adopt Digital Health Tools
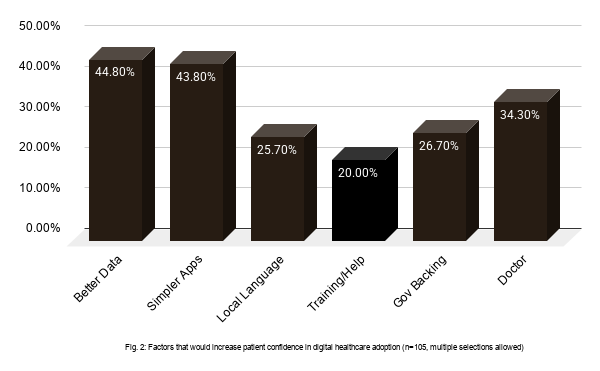
Source: DHN Bureau Patient Survey 2026
When patients were asked what would make them adopt digital health tools more confidently, their answers were not abstract. Better data privacy assurance leads at 44.8%, a direct echo of the concerns chart above, and a clear signal that the barrier and its solution are two sides of the same coin. Simpler apps follow at 43.8%, separated from the top response by a single percentage point, meaning usability and trust are essentially tied as the two things patients most want fixed. Together, these two responses alone account for nearly 9 in 10 respondents selecting them. Doctor recommendation, at 34.3%, is perhaps the most strategically underused lever in the room. Patients are far more likely to trust a digital tool when their physician endorses it, yet most platforms still acquire users through marketing rather than clinical champions.
Government backing (26.7%) and local language support (25.7%) speak to legitimacy and inclusion, respectively. Patients want to know the system is regulated and that it speaks their language, literally. The chart, read as a whole, is a sequenced action plan. Fix privacy, simplify the experience, get doctors to recommend it, and make it work in every Indian language. The patients have done the strategy work. The question is whether the industry is ready to execute it.
One respondent from a Tier 3 setting described a scenario that encapsulates the paradox perfectly: a patient was able to receive specialist care via video call without traveling to a distant city hospital, a genuine win for access. But poor internet connectivity caused the call to drop repeatedly, ultimately forcing the patient to make that journey anyway.
For healthcare startup founders and hospital leaders, the Tier gap presents both a responsibility and an opportunity. Designing for the metro user first and retrofitting for rural later is a strategy that has consistently failed. The solutions, vernacular interfaces, offline-first design, community health worker integrations, USSD-based fallbacks, are known. What is missing is the business will to prioritize them.
Where We Can Do Better: Three Clear Signals from Patients
Across open-ended responses, patients were remarkably specific about what would make them adopt digital healthcare more confidently. Better data privacy assurance was the most requested enabler, mentioned across age groups and tiers. Patients want transparency about who accesses their data, how it is stored, and what recourse they have. DPDP Act implementation in healthcare contexts will matter, but patients want to feel it.
Simpler apps and interfaces followed closely. Multiple respondents described getting stuck, logging out unexpectedly, failing OTP cycles, or not knowing how to navigate from one section to another. Usability is a clinical issue; a patient who cannot access their lab report is effectively unserved. As one respondent put it: "Struck and loading."
Local language support appeared consistently, particularly from Tier 2, Tier 3, and some metro respondents. The default assumption that English-language interfaces are universally accessible is incorrect and exclusionary. Healthcare communication must meet patients in their language, not the other way around.
Beyond these three, patients also cited the need for better staff training to guide digital tool navigation, greater government backing for legitimacy and scale, and stronger doctor recommendations as a trust catalyst. Notably, when a doctor recommends a digital tool or platform, patient adoption increases significantly. This suggests that physician champions are an underutilized lever in digital health onboarding.
The Readiness Question
We asked every respondent a direct question: Is Indian healthcare ready for full digital transformation?
The answers were, predictably, divided, but the reasoning behind them was far more unified than the conclusions. Those who said "yes" typically qualified it: "Metro cities are full-fledged to move, but Tier 1 and 2 are not." Those who said "not yet" pointed to the same set of gaps: digital literacy, data trust, connectivity, and language access.
Very few respondents were categorically opposed to digital health. Most positioned themselves as conditional advocates, willing to embrace digital tools when those tools are trustworthy, accessible, simple, and connected to the physical care they still value.
For digital healthcare leaders, hospital executives, and startup founders, this survey offers a clear message: the infrastructure argument is being won. Patients know what apps are, they have used digital payments, and they have received their blood work on WhatsApp. The next frontier is relational and patient-centric. It is about building trust, language bridges, clinical confidence, and equitable access that will turn early adopters into advocates and skeptics into participants.
And the patients have, in this survey, been generous enough to tell us exactly what they need.
The question is whether we are listening.
Disclaimer
This survey was conducted primarily through a self-administered digital questionnaire, which may introduce self-selection bias toward respondents with existing digital access and literacy. The sample, while cross-tier and cross-generational, is not statistically representative of India's 1.4 billion population, and findings should be interpreted as indicative rather than definitive. Rural and elderly populations, who are arguably the most critical cohorts for equity-focused digital health policy, may be underrepresented relative to their actual numbers. Future research with larger sample sizes, community-based recruitment methods, and multilingual data collection instruments would strengthen these findings considerably.
Stay tuned for more such updates on Digital Health News